and move towards health
Misdiagnosis of CFS -
Chronic Fatigue Syndrome
A misdiagnosis of CFS is a natural concern for any of us diagnosed with Chronic Fatigue Syndrome (CFS) or Myalgic Encephalomyelitis (aka M.E).
This CFS article is for you if you are asking or saying:
- "What if I have a different illness than Chronic Fatigue Syndrome?"
- "Could a different chronic illness be the cause of CFS symptoms?"
- "I want to check that I am not misdiagnosed with CFS, because I worry that there is a treatment out there that I could be getting."
Or click here to CHOOSE FROM
A RANGE OF personalizable cards and gifts.
The healing-themed gifts are designed by myself, Katherine, the author of
this website HealingCFSME.com
Proceeds go towards the cost of the website. Thank you. Enjoy!
In these two CFS articles (also ME), I give a list of other chronic illnesses with some overlapping
symptoms to those of CFS.
For some or them, tests and treatment are available.
Please note that there are other illnesses and conditions which should have been excluded before a diagnosis of Chronic Fatigue Syndrome was given.
Your medical practitioner should have arranged neurological tests and blood tests. Possibly you will have been given an EEG, an ECG and even a MRI scan.
For many of the conditions or chronic illnesses listed here, as for CFS, alternative healing methods are the only
treatments available. If there is no additional treatment, there may be little advantage to
receiving another diagnosis.
If you haven't done so already, you may find that your energy-time is better allocated to getting the basics in place to manage your health.
Why is there a risk of misdiagnosis of CFS?
For the following reasons a misdiagnosis of CFS Chronic Fatigue Syndrome or Myalgic Encephalomyelitis is possible.
- Some/many view CFS as a misdiagnosis in the first place. The expert Dr Jacob Teitelbaum says he takes 3 minutes to diagnose CFS or Fibromyalgia. And the next 3 hours to narrow down the diagnosis to one of over one hundred possible causes that contribute to this cluster of symptoms. This suggests that his conclusion after 3 hours IS the diagnosis. Some of that one hundred causes are no doubt listed in these two CFS articles.
- Currently Chronic Fatigue Syndrome causes are not known, despite the fact that the illness affects over
250, 000 people in the UK alone. - The risk of misdiagnosis is increased by a lack of agreement about the symptoms needed to reach a diagnosis of CFS.
- Chronic fatigue (not the syndrome) is a symptom of many different illnesses. It can sometimes be resolved
fairly easily, for example if lack of sleep, hypoglycemia, or poor
nutrition are responsible.
There is a risk that someone presenting with chronic fatigue may incorrectly be given a Chronic Fatigue Syndrome diagnosis. - As long
as there is no blood test or other clear diagnostic marker for this
chronic illness, there is a risk of misdiagnosis of CFS - Chronic Fatigue Syndrome.
Contents for this article on Have I been Misdiagnosed with Chronic Fatigue Syndrome?
- Chronic Illnesses to exclude when asking if you have been misdiagnosed with Chronic Fatigue Syndrome
- Diet related conditions which can lead you to be misdiagnosed with CFS
Move here for a further CFS/ME article which includes the following:
- Deficiencies that can lead to a potential misdiagnosis of Chronic Fatigue Syndrome
- Environmental cause leading to a potential misdiagnosis of CFS
- Other issues to exclude as a cause of fatigue and other symptoms
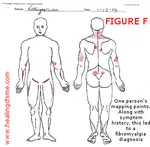
A chronic illness with overlapping symptoms may lead to misdiagnosis of CFS
Chronic Illnesses to exclude when considering a diagnosis of Chronic Fatigue Syndrome include the following:
- Adrenal Fatigue
It is unclear if adrenal fatigue is the same thing as a Chronic Fatigue Syndrome diagnosis or something different.
Those with adrenal fatigue often talk of having burned out and seem less likely than those with CFS/ME to talk of an illness as being the trigger. The only treatment is through complementary healing methods. - Addison disease is an adrenal disorder which may follow extreme physical training over an extended period. The adrenal gland shuts down totally and can be life-threatening.
It is treatable through continual replacement of corticosteroids. - Ehlers-Danlos (EDS)
Consider Ehlers Danlos if your joints are hyper mobile and you bruise easily.
There may be a link between EDS and Mast Cell disorders. - Mast Cell Activation Syndrome
Mast Cell Activation Syndrome is a term used increasingly from around 2010. The symptoms appear to overlap with those of allergy. Please do your own research. It appears that testing is possible.
Investigate Mast Cell Activation if you have sleep problems, allergies and brain fog.
Also "histamine can mimic symptoms of anxiety and trigger depression and other psychiatric conditions"
Quote from... https://healinghistamine.com/how-histamine-affects-sleep/
Research from... https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3753019/
The person I have heard talk about Mast Cell Activation treatment is Beth O'Hara.
She recovered from being severely ill with mast cell activation syndrome, histamine intolerance, Lyme, mold toxicity, fibromyalgia and chronic fatigue.
The treatment is available in the USA only. Look for https://mastcell360.com.
A survey is available on that website for anyone who wants to know if Mast Cell Activation is relevant to them. - Lyme Disease
Consider Lyme disease if you might have been bitten by a tick.
Katina Makris wrote the book Out Of The Woods about her experience with a long-term illness at one point diagnosed as Chronic Fatigue Syndrome which turned out to be Lyme disease.
Her re-diagnosis with Lyme disease didn't lead to any quick or easy solution, but as a result of treating it with complementary / alternative healing methods, she is back on her feet again. -
Non radiographic axial
spondyloarthritis
If the extreme tiredness or fatigue is accompanied by back pain and stiffness then consider a diagnosis of ankylosing spondylitis.
The condition often first appears in teenagers and young adults. It’s twice as common in men.
Symptoms are likely to be better after exercise rather than worse.
Tests are available for ankylosing spondylitis – blood tests and MRI tests.
However, there is a related earlier stage to this illness called non radiographic axial spondyloarthritis. This diagnosis is much harder to spot in the MRIs until the point when fusion takes place. Fusion takes place quite quickly. Thus the risk of a possible misdiagnosis of CFS chronic fatigue syndrome.
Doctors are likely to know about ankylosing spondylitis. They are less likely to know about non radiographic axial spondyloarthritis which can proceed it. -
Porphyria
Porphyria is a genetic condition.
Some with porphyria could have been misdiagnosed with CFS/ME
Possible overlapping symptoms include: limb weakness and abdominal pain, nausea, severe diffuse pain, insomnia, or anxiety.
An adverse reaction to sunlight can suggest porphyria.
Diagnosis: Porphyria is revealed by a blood, urine, or stool test, preferably at or near the time of symptoms which may be variable. - SIBO stands for Small intestinal bacterial overgrowth. The condition affects the small intestine when
bacteria that should grow in other parts of the gut start grow there. It is often seen as overlapping with a CFS diagnosis. The treatment is antibiotics.
- Sjögren's Syndrome
Consider Sjögren's if you experience dry eyes. Even if you don't have Sjögren's Syndrome you might like to check out this article on foods that help dry eyes.
I know someone who had an operation for Sjögren's and recovered her energy.
Dry eyes can also be a symptom of health problems due to mould exposure. - Depression
Depression is a serious condition. It is often accompanied by chronic fatigue, but not by the full range of symptoms of CFS.
I have met two men who thought they had CFS/ME but recovered their energy within a year and concluded that they had had depression.
However, depression is commonly experienced by people with CFS/ME, so you can have both. I consider depression to be a frequent consequence or symptom of CFS/ME.
If you have depression on its own, then it may help to increase your level of exercise. If your depression is relieved by exercise, then you don't have the key Chronic Fatigue Syndrome symptom of post-exertional malaise.
- Chronic Pain Syndrome (Type #CPS to find Chronic Pain Syndrome sufferers on twitter).
I am not clear yet if the presence of Chronic Pain Syndrome indicates a misdiagnosis of CFS or if this is potentially a diagnosis you might have in addition to one of CFS. Please note that chronic pain is a common symptom of Chronic Fatigue Syndrome or Myalgic Encephalomyelitis.
There is no clear treatment protocol for Chronic Pain Syndrome. -
Myasthenia Gravis
Weakness is a key symptom of Myasthenia Gravis and might lead to misdiagnosis of CFS or Myalgic Encephalomyelitis. Blood tests and treatment are available.
Symptoms can include a drooping of one or both eyelids, difficulty in swallowing, a changed facial expression, double or blurred vision, unstable walking, shortness of breath, impaired speech (dysarthria), and weakness in the arms, hands, fingers, legs, and neck. - Postural orthostatic tachycardia syndrome
( PoTS)
Why do I feel dizzy when I stand up?
Again this is often an overlapping condition rather than a misdiagnosis of CFS. Studies from both the UK and Australia indicate that PoTS is found in up to one third of people with ME /CFS.
Consider PoTS if you are usually dizzy when you stand up and even possibly when you are lying down (- I used to be!) PoTS is due to your heart rate increasing by 30 beats per minute as you stand up.
Alternatively dizziness on standing can be due to a drop in blood pressure - this is called orthostatic hypotension. Dizziness is also a common symptom of hypoglycemia.
The cause of PoTS is not known. Ask your medical practitioner if any treatment is available. Visit www.potsuk.org for more information. - Multiple Sclerosis
A friend's diagnosis was changed from Myalgic Encephalomyelitis to Multiple Sclerosis. Many symptoms overlap, including chronic fatigue. - Undifferentiated Connective Tissue Disease (UCTD)
Possible symptoms include aching joints, low grade fever, dry eyes, and a rash in response to being out in the sun. Someone has advised me that she was misdiagnosed as CFS and was later diagnosed with UCTD. However, fatigue is not listed as a symptom. Please do your own research. You can read more about UCTD here.
Diet related conditions which can lead to a potential misdiagnosis of Chronic Fatigue Syndrome
It is well worth checking to see if a change to your diet can relieve the symptoms of Chronic Fatigue Syndrome.
- Is a problem with a food causing symptoms and chronic illness?
* Food allergies
Food allergies can be tested for.
* Food sensitivities
I know someone who cut out various foods and has experienced recovery from CFS /ME as a result
- Coeliac disease
People with coeliac disease are tired all the time because they are not absorbing nutrients from the food. They experience amazing relief from cutting out gluten to which they are intolerant. Coeliac disease often goes undiagnosed. There is a test for coeliac disease. Food allergies and food sensitivities
Both food allergies and food sensitivities can cause serious symptoms including chronic fatigue.
With a food sensitivity you may not notice feeling worse after eating a certain food. - Hypoglycemia
Consider hypoglycemia if you need to eat frequently and experience dizziness if you do not eat frequently. Reactive hypoglycemia is often a symptom not a cause of Chronic Fatigue Syndrome. Hypoglycemia is a prevalent symptom for people with CFS/ME. It is well worth adjusting your eating patterns to see if you experience relief. - Aspartame poisoning
If you drink a lot of fizzy drinks or sodas, consider aspartame poisoning. - Leaky Gut Syndrome or intestinal permeability and Irritable Bowel Syndrome
Leaky Gut is often mentioned by alternative practitioners. The NHS is unconvinced by this health label and unconvinced by the claims made for diets that can help.
In contrast, the NHS take Irritable Bowel Syndrome IBS seriously and offers advice.
https://www.nhs.uk/conditions/irritable-bowel-syndrome-ibs/
Consider that you may have IBS, and therefore a misdiagnosis of CFS, if fatigue is accompanied by bloating, diarrhoea, constipation and stomach cramps.
Advice for gut health includes eating fermented foods like kefir and avoiding unnecessary antibiotics.
Wishing you health both within and beyond illness,
Katherine
Katherine T Owen runs this website - www.HealingCFSME.com.
She is author of the booklet of 15 poems, Be Loved, Beloved
(Read it in paperback at lulu.com or on kindle)
- Click through to read part two of Possible Misdiagnosis of Chronic Fatigue Syndrome/ME.
- The cause of Chronic Fatigue Syndrome and Myalgic Encephalomyelitis is not known. Nonetheless, those of us living with the illness often get asked the question: What is the cause of CFS?
Click through to read some suggestions of how to answer this question. - Or click on the link below to move from Do I have a Misdiagnosis of CFS? to read about the criteria and symptoms which are necessary for a diagnosis of CFS.
- Home Page
- CFS/ME Diagnosis
- What else could CFS be?
Receive daily inspiration...
by putting your favorite (favourite) healing quote on
a mug, cushion, postcard, coaster, T shirt etc.
You will find my zazzle gift store at
zazzle.com/HealingStore.
Use one of my designs or start from a blank.
Thank you from me, Katherine, author of HealingCFSME.com
 |
© Katherine T Owen. All articles on this website are copyrighted. I am delighted if you choose to click above to share this page on social media, but please
do not copy, print or otherwise use without my permission. Thank you. Disclaimer:
I am not a medical practitioner. The articles on this website are not
to be taken as medical advice. Please consult a medical practitioner as
necessary. |